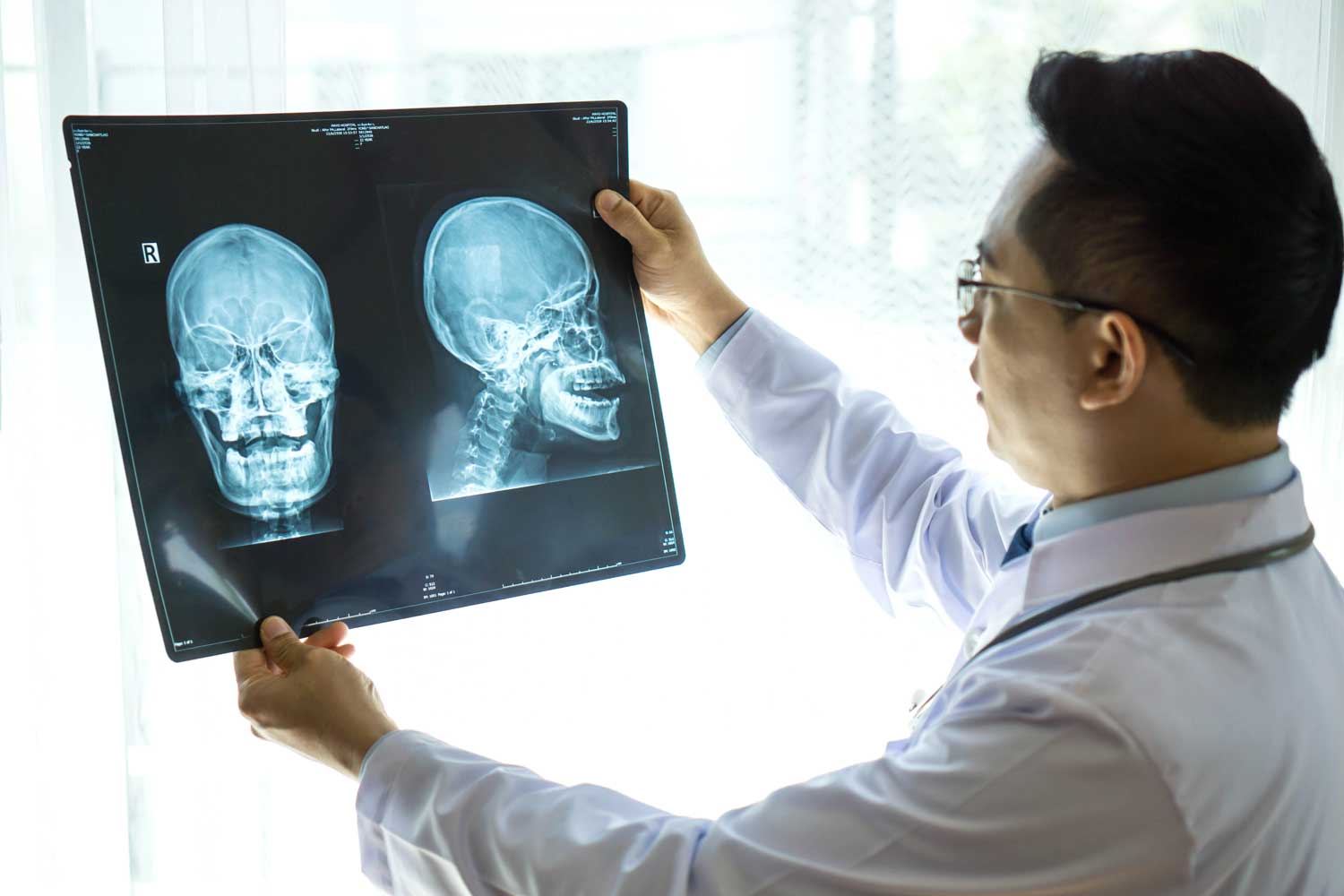
A skull X-ray produces detailed images of the bones of the cranial vault and facial skeleton, allowing your doctor to evaluate fractures, bone lesions, calcifications, and structural abnormalities of the skull. While CT and MRI have largely replaced skull X-rays for head trauma and intracranial evaluation, the skull X-ray retains an important role in specific clinical situations — including the assessment of metabolic bone disease, the initial evaluation of low-risk head injuries, part of skeletal surveys for conditions like multiple myeloma, and medicolegal documentation.
At Independent Physicians Medical Center (IPMC) in Northeast Philadelphia, we provide advanced digital skull X-ray imaging using the Siemens Multix system, with results typically available within 24 to 48 hours and sent directly to your referring physician. Learn more about our X-ray services.
What Does a Skull X-Ray Show?
The skull is composed of 22 bones — 8 forming the cranial vault (the bony shell that protects the brain) and 14 forming the facial skeleton. A skull X-ray evaluates:
- The cranial vault bones — the frontal, parietal, temporal, and occipital bones, including their outer and inner tables and the cancellous diploic space between them
- Skull sutures — the fibrous joints between cranial bones (coronal, sagittal, lambdoid sutures); sutures must be distinguished from fracture lines, which can be challenging
- Vascular channels — grooves from meningeal arteries (especially the middle meningeal artery) are normally visible and must be distinguished from linear fractures
- Bone density and thickness — diffuse or focal changes in skull bone density may indicate metabolic disease, metastases, or Paget’s disease
- Intracranial calcifications — the pineal gland, choroid plexus, dura, and certain pathological lesions can calcify and become visible on skull X-ray
- Foreign bodies — dense metal fragments or certain types of glass embedded in the scalp or skull
Common Conditions a Skull X-Ray Diagnoses
Skull fractures. A skull X-ray can detect linear and depressed fractures of the cranial vault. Linear fractures appear as thin, dark, straight or branching radiolucent lines crossing the skull — they must be distinguished from the normal vascular grooves (which have a halo of increased density around them) and sutures (which follow predictable anatomical locations and have a saw-toothed appearance). Depressed fractures appear as areas of increased density where fractured bone fragments overlap.
An important limitation: skull X-ray is poor at detecting skull base fractures (fractures through the floor of the skull), which are often diagnosed clinically by signs such as Battle’s sign (bruising behind the ear), raccoon eyes, or CSF leaking from the nose or ear. For any significant head injury with suspected intracranial complications, a CT scan of the head is the investigation of choice — it shows not only fractures but also bleeding and brain injury that are completely invisible on plain X-ray.
Multiple myeloma. Multiple myeloma is a plasma cell cancer that destroys bone, producing characteristic “punched-out” lytic (dark, round, well-defined) lesions throughout the skeleton — most visibly in the skull, where their profusion gives the classic pepper-pot skull appearance on the lateral view. A skull X-ray is traditionally part of the skeletal survey used to stage and document myeloma bone disease, though whole-body low-dose CT is now increasingly preferred as the standard of care for its greater sensitivity in detecting smaller lesions.
Paget’s disease of bone. Paget’s disease is a metabolic bone disorder causing excessive, disorganized bone remodeling — common in people over 50. The skull is one of the most frequently affected bones. Early Paget’s in the skull produces a large area of lysis (called osteoporosis circumscripta), characteristically involving the frontal or occipital bone. Later stages produce a mixed pattern of lysis and dense sclerosis — multiple irregular white patches against a darker background, described as a cotton-wool appearance — alongside thickening and expansion of the skull vault. These findings are often distinctive enough to be diagnostic on plain X-ray.
Bone metastases. Cancer that has spread to the skull from a primary tumor elsewhere (commonly breast, lung, prostate, kidney, thyroid) can produce lytic or sclerotic lesions in the skull vault. Lytic metastases (from breast cancer, lung cancer, kidney cancer) appear as dark, rounded areas of bone destruction; sclerotic metastases (from prostate cancer) appear as areas of increased whiteness. Skull X-ray may identify these lesions but CT or MRI is more sensitive and provides better characterization.
Intracranial calcifications. Calcification of the pineal gland is a normal finding in adults and is visible on skull X-ray as a small, dense midline dot. Importantly, the pineal gland normally sits in the midline; if it appears shifted to one side on the AP view, this was historically a sign of an expanding intracranial mass pushing it off-center. Today, CT or MRI has replaced skull X-ray for this purpose entirely. Pathological calcifications — in meningiomas, craniopharyngiomas, tuberous sclerosis, and certain infections — may also be visible.
Congenital and developmental abnormalities. Skull X-ray can demonstrate abnormal head shape, premature fusion of skull sutures (craniosynostosis), and other structural variants. In children, the patency and width of the fontanelles and sutures are assessed.
Foreign bodies. Metal fragments, dense glass, and other radio-opaque objects embedded in the scalp or skull vault are visible on plain X-ray. Organic materials such as wood are not visible and require ultrasound or MRI for detection.
When Does a Doctor Order a Skull X-Ray?
The indications for skull X-ray have narrowed considerably since CT became widely available — for most head injuries and neurological evaluations, CT is the first-line choice. However, a skull X-ray is still appropriately ordered when:
- A skull fracture is suspected after a low-energy head impact in a stable patient, particularly when CT is not immediately indicated by clinical criteria but documentation or further reassurance is needed
- Multiple myeloma is suspected or known — as part of a complete skeletal survey to document and stage bone involvement
- Paget’s disease of the skull is suspected — a skull X-ray can be diagnostic
- Bone metastases to the skull vault are suspected or need to be documented
- An abnormal head shape or suspected craniosynostosis needs initial assessment
- A foreign body is suspected in the scalp or skull
- Medicolegal documentation of a head injury is required
- Baseline imaging before or after skull surgery
According to Johns Hopkins Medicine, skull X-rays are used less frequently today due to the superior diagnostic capabilities of CT scanning, particularly for head trauma — though they remain a useful, low-cost, low-radiation tool in specific clinical contexts.
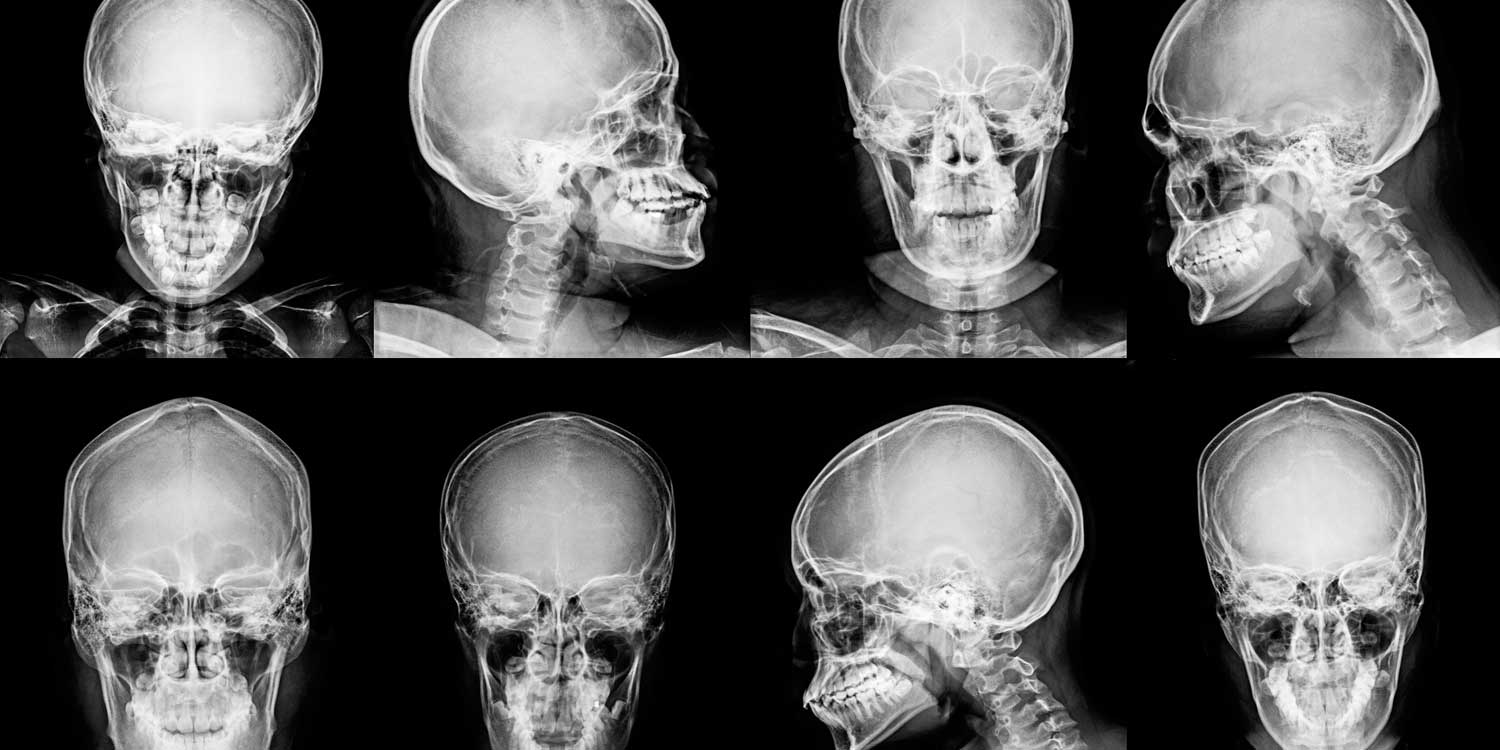
The lateral skull X-ray is the most informative single projection, showing the cranial vault, sutures, vascular channels, sella turcica, and skull thickness — and is the best view for detecting linear fractures and the characteristic bone changes of Paget’s disease and myeloma.
Standard Views — What Each Reveals
A standard skull series typically includes two to four views. Each is angled to project different parts of the skull without overlapping structures obscuring the detail.
The lateral view is the single most informative projection of the skull and is always included. The patient’s head is turned 90 degrees so the beam passes through one side to the other. It provides an excellent side-profile view of the entire cranial vault, sutures (coronal, lambdoid, sagittal), the sella turcica (the saddle-shaped bony seat of the pituitary gland), and vascular channels. The lateral view is best for detecting linear fractures of the parietal and temporal bones, visualizing the frontal and sphenoid sinuses, and assessing skull thickness and density for conditions like Paget’s disease or myeloma.
The PA (posteroanterior) or Caldwell view is taken with the face directed toward the detector. It provides a frontal view of the skull and shows the frontal bone, orbits, nasal bones, and the relationship of the cranial midline structures. On this view, pineal gland displacement from midline can be assessed and frontal sinus abnormalities are visible.
The Towne’s view (also called the AP axial view) is taken with the beam angled downward from the front, projecting the occipital bone and the foramen magnum forward and free of overlapping structures. It is particularly useful for visualizing the posterior fossa, the occipital bone, the internal occipital protuberance, and the petrous ridges. It is the best view for fractures involving the occipital bone or the posterior vault.
Additional views — including a submentovertex (base view) for the skull base, and oblique projections — may be requested in specific situations. Your referring physician or radiologist will indicate which views are most appropriate for your clinical question.
The Critical Limitation: Why CT Is Often Needed for Head Injuries
For patients presenting with significant head injury, a skull X-ray alone is insufficient and can be misleading. There are two fundamental problems.
First, a skull X-ray shows only the bone — not the brain. A patient can have a devastating intracranial injury (subdural haematoma, extradural haematoma, brain contusion) with no fracture visible on X-ray. Conversely, a linear skull fracture on X-ray can look alarming but carry no intracranial injury. The fracture itself is rarely the clinical problem — it is the intracranial consequences that determine clinical management and prognosis.
Second, skull X-rays miss a significant proportion of fractures. Basal skull fractures (through the floor of the skull) are rarely visible on plain films and are usually diagnosed clinically. A CT scan of the head evaluates both the bone and the brain in a single study, making it the standard of care for any head injury with loss of consciousness, focal neurological symptoms, persistent headache, vomiting, or mechanism suggesting high energy.
If your doctor has ordered a skull X-ray for a head injury, it is because they have already assessed your clinical risk and determined that CT is not currently indicated — or the X-ray is for documentation or low-energy trauma assessment purposes. If there is any clinical concern for intracranial injury, CT is requested.
How to Prepare and What to Expect
A skull X-ray requires no preparation at all. You can eat, drink, and take your medications as normal. For complete guidelines, see IPMC’s X-ray preparation page.
When you arrive, you will be asked to remove all metal from your head, neck, and ears — earrings, necklaces, hair pins, barrettes, and hearing aids — as these create bright artifacts that can obscure skull structures. You should also remove glasses. Dental metalwork inside the mouth can cause minor artifacts but does not require removal.
You will sit or lie on the X-ray table while the technologist precisely positions your head for each view. Your head will be in different positions for each exposure — turned to the side for the lateral view, facing forward for the PA view, tilted back for the Towne’s view. For each exposure, you must stay completely still for a fraction of a second. Any movement blurs the image and may require a repeat.
The exam takes approximately 10 to 15 minutes and is entirely painless. If your head injury makes positioning uncomfortable, the technologist will work carefully to minimise movement.
Pregnancy: always inform the technologist if you are or may be pregnant. The skull X-ray directs the beam through the head — scatter to the abdomen is extremely low for this study, and when clinically indicated, the exam can generally be performed safely.
After Your Skull X-Ray: Results and Next Steps
A board-certified radiologist at IPMC reviews every image and prepares a detailed written report for your referring physician, typically within 24 to 48 hours. Your doctor will explain what the findings mean and what next steps are appropriate.
Depending on what the X-ray shows, your doctor may:
- Reassure you that no fracture or significant abnormality is present
- Request a CT scan of the head for definitive fracture characterization or to evaluate the brain if any intracranial concern exists
- Order an MRI of the brain for detailed evaluation of intracranial structures, suspected tumors, or soft tissue lesions invisible on X-ray
- Refer to a haematologist or oncologist if myeloma or metastatic bone disease findings are identified
- Arrange further metabolic bone disease evaluation (bone scan, additional blood tests, rheumatology referral) if Paget’s disease is found
- Schedule follow-up imaging at an interval to monitor a known condition
X-rays at IPMC
Why Choose IPMC for Your Skull X-Ray in Philadelphia?
Advanced Digital Imaging with the Siemens Multix
IPMC uses the Siemens Multix — a state-of-the-art digital radiography system that delivers sharp, high-resolution skull X-ray images with minimal radiation. Digital acquisition provides immediate image availability for radiologist review and easy comparison with prior studies.
Board-Certified Radiologists
Every skull X-ray is interpreted by a board-certified radiologist experienced in skeletal and neurological imaging. Detailed reports — covering fracture assessment, bone density changes, lesion characterization, and recommendations for follow-up imaging — are sent directly to your referring physician within 24 to 48 hours.
Fast Appointments, No Hospital Wait Times
Most skull X-ray appointments at IPMC are completed in about 10 to 15 minutes. Same-day and next-day scheduling is often available. Get your imaging quickly, without the delays and complexity of a hospital radiology department.
Convenient Location and Flexible Hours
Located at 9908 E. Roosevelt Blvd. in Northeast Philadelphia with onsite parking. Open Monday–Friday, 8AM–8PM. We accept most major insurance plans.
Schedule Your Skull X-Ray at IPMC in Philadelphia
If your doctor has recommended a skull X-ray in Philadelphia, IPMC provides fast, digital imaging in a comfortable outpatient setting in Northeast Philadelphia — with results delivered directly to your physician.
- Call 215-464-3300 to schedule your appointment.
- 9908 E. Roosevelt Blvd., Philadelphia, PA 19115
- Monday–Friday, 8AM–8PM