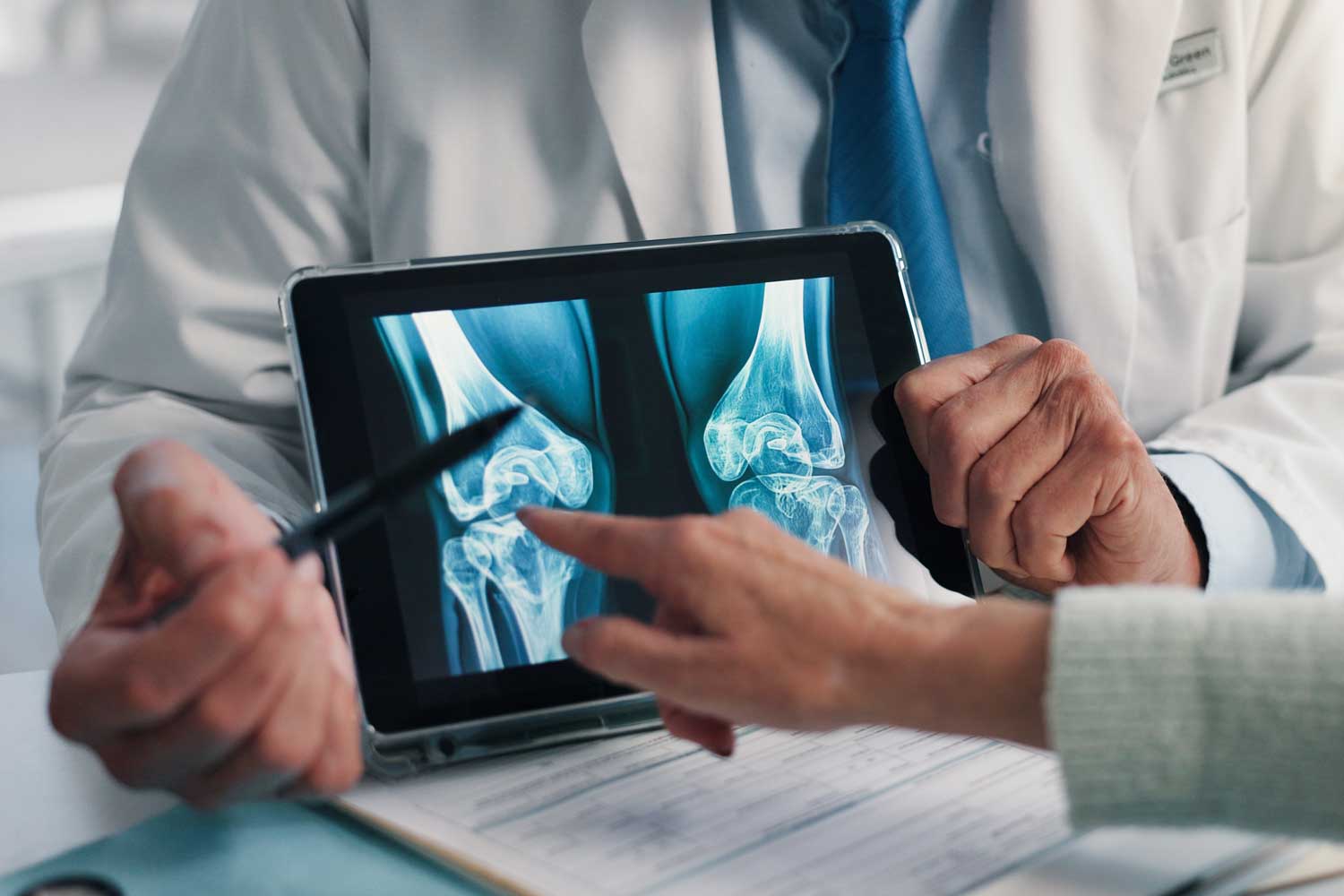
Knee osteoarthritis (OA) is one of the most common causes of chronic pain and disability, particularly in middle-aged and older adults. When your doctor suspects arthritis behind your knee pain, a knee X-ray is the standard first imaging test — fast, affordable, and highly informative. It reveals the structural hallmarks of cartilage loss, grades the severity with an established scoring system, and provides the documented evidence doctors and insurers need to guide treatment decisions from conservative management through to surgical planning.
At Independent Physicians Medical Center (IPMC) in Northeast Philadelphia, we provide advanced digital knee X-ray imaging using the Siemens Multix system — including the critical weight-bearing views that give the most accurate picture of knee joint health. Learn more about our X-ray services.
What Knee Osteoarthritis Looks Like on X-Ray
Osteoarthritis is a degenerative condition in which the cartilage cushioning the joint surfaces gradually breaks down over time. Because cartilage is not visible on X-ray, its loss is assessed indirectly by the space between the bones. As cartilage wears away, the gap between the femur (thighbone) and tibia (shinbone) narrows — and eventually disappears entirely in severe disease, producing bone-on-bone contact. A knee X-ray reveals four classic hallmarks of this process.
Joint space narrowing is the primary marker of cartilage loss. Radiologists assess the joint space in each of the three knee compartments: the medial (inner) compartment between the femur and tibia on the inside of the knee (the most commonly affected area), the lateral (outer) compartment, and the patellofemoral compartment between the kneecap and the front of the femur. Weight-bearing X-rays are essential here — non-weight-bearing images can make arthritic joints look better than they are, as the normal load on the knee is what drives the bones together and reveals the true extent of cartilage loss.
Osteophytes (bone spurs) are bony projections that form at the margins of the joint surfaces and the attachment points of ligaments and tendons as the body attempts to stabilize a worn joint. Osteophytes are a hallmark of OA and become more prominent as the disease advances. They can sometimes cause mechanical symptoms — catching, locking, or restricted range of motion — if they grow large enough to interfere with joint movement.
Subchondral sclerosis is increased density (whitening) of the bone just beneath the joint surface. When cartilage is lost, the underlying bone absorbs more compressive load than it was designed to, and it responds by becoming denser. This appears as a bright white band running along the joint surface on the X-ray.
Subchondral cysts are small fluid-filled cavities that form in the bone beneath the arthritic joint surface. They appear as small round lucent (dark) areas just below the dense white sclerotic band and indicate significant joint loading and bone remodeling.
In advanced disease, the joint may show malalignment as well — varus deformity (“bowlegged”) from medial compartment collapse, or valgus deformity (“knock-kneed”) from lateral compartment collapse. These alignment changes are visible on the standing AP view and have important implications for surgical planning.
The Kellgren-Lawrence Grading System: Staging Your Arthritis
When a radiologist interprets a knee X-ray for arthritis, they assign a Kellgren-Lawrence (KL) grade — a standardized severity score from 0 to 4 that has been used worldwide since its development in 1957. This grade appears in your radiology report and gives your doctor (and insurer) a consistent, documented measure of how much arthritis is present. Many insurance providers require a specific KL grade to authorize certain treatments, including total knee replacement.
| KL Grade | Severity | X-Ray Findings | Typical Clinical Picture |
|---|---|---|---|
| 0 | Normal | No features of osteoarthritis. Normal joint space. No osteophytes. | No OA present radiographically. Symptoms, if any, from other causes. |
| 1 | Doubtful | Possible small osteophytes of doubtful significance. No definite joint space narrowing. | Mild or no symptoms. Early changes — may represent the beginning of degenerative change. Important window for preventive lifestyle intervention. |
| 2 | Mild | Definite osteophytes. Possible (but not definite) joint space narrowing. | Symptoms may be mild or absent. Cartilage deterioration is beginning. Best window for conservative treatment to slow progression. |
| 3 | Moderate | Multiple osteophytes. Definite joint space narrowing. Subchondral sclerosis. Possible deformity of bone ends. | Chronic knee pain, stiffness, and reduced function. Conservative treatment remains the first-line approach, but symptoms are often significant. |
| 4 | Severe | Large osteophytes. Severe joint space narrowing (often bone-on-bone). Marked subchondral sclerosis. Definite bone deformity. | Significant pain, loss of function, and often deformity. Surgical consultation for knee replacement is commonly discussed at this stage. |
An important caveat: the KL grade on X-ray does not always predict how much pain or disability a patient experiences. Some patients with KL Grade 4 changes function reasonably well; others with KL Grade 2 changes have significant symptoms. Your doctor considers the X-ray findings alongside your clinical history, symptoms, function, and goals when making treatment decisions — the grade is a tool, not a verdict.
Three Knee Compartments: Why Location Matters
The knee is divided into three distinct compartments, and OA does not always affect all three equally. Understanding which compartment is most affected guides both non-surgical treatment and surgical options.
The medial (inner) tibiofemoral compartment is the most commonly affected by OA, accounting for the majority of symptomatic knee arthritis. Medial compartment narrowing causes a varus (bowlegged) alignment deformity as the inner knee collapses. Most patients with significant medial OA will note pain along the inner aspect of the knee.
The lateral (outer) tibiofemoral compartment is less commonly the primary site of OA but is frequently involved in combination with medial disease. Isolated lateral compartment OA can produce a valgus (knock-knee) deformity.
The patellofemoral compartment between the kneecap and the front of the femur is a separate source of knee pain, particularly with activities that load the front of the knee — stairs, squatting, kneeling, and rising from a chair. Patellofemoral OA is best evaluated on the sunrise (skyline) view, which profiles the kneecap joint directly.
Bilateral knee OA (arthritis in both knees) is very common and is assessed with standing X-rays of both knees taken together for comparison. Comparing left and right sides reveals whether the disease is symmetric or asymmetric — important when planning surgical timing.
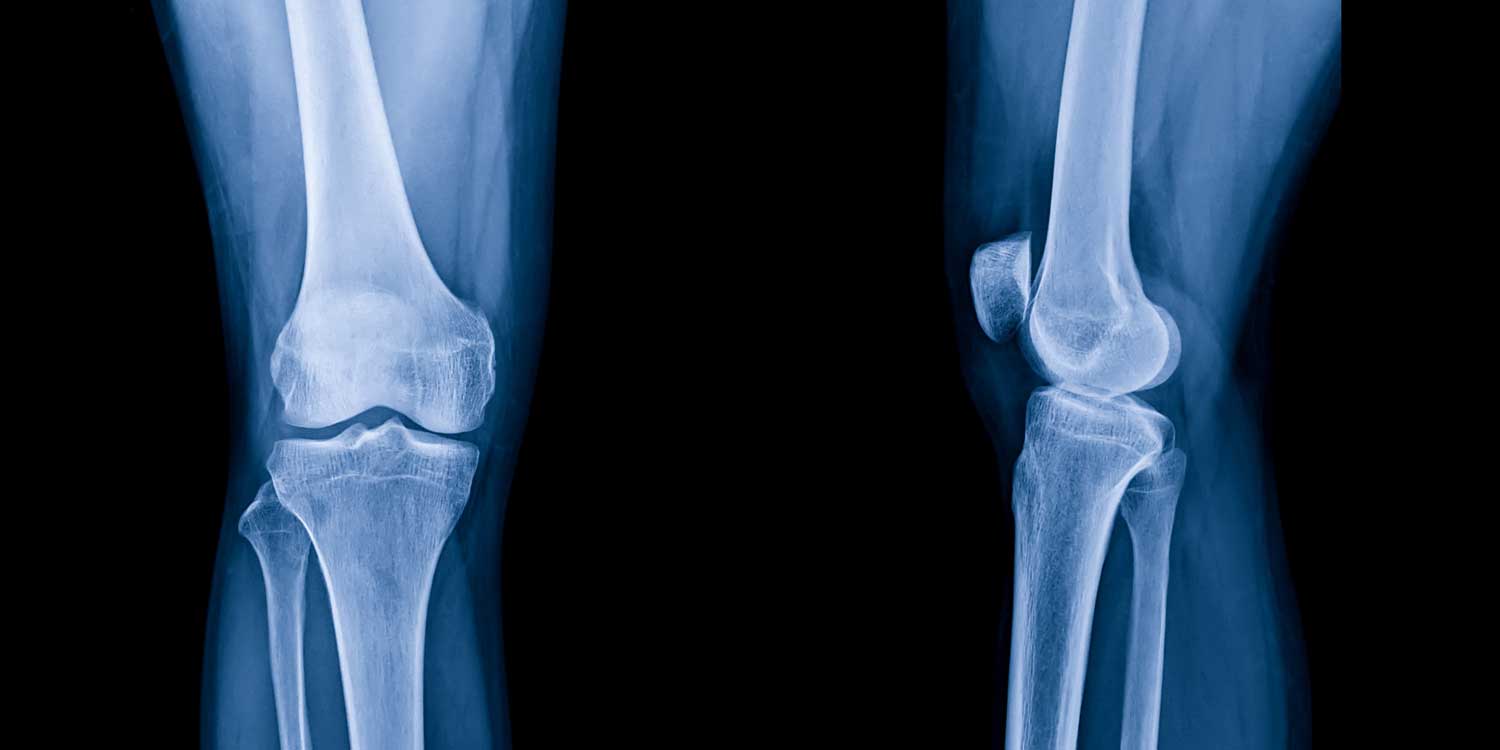
A weight-bearing AP knee X-ray shows the medial and lateral tibiofemoral compartments under real physiological load — the most accurate view for assessing joint space narrowing and assigning a Kellgren-Lawrence grade.
Why Weight-Bearing X-Rays Are Essential
A knee X-ray for osteoarthritis assessment must be taken while the patient is standing with full weight on the knee. This is called a weight-bearing (standing) X-ray, and it is the recommended technique for arthritis evaluation for a critical reason: when you are lying down, the compressive load on the knee joint is removed, and the joint space may look normal or near-normal even in moderately arthritic knees. Standing under your body’s weight approximates the real conditions under which cartilage loss has occurred — and reveals the true joint space.
Non-weight-bearing X-rays significantly underestimate the degree of joint space narrowing and can result in under-grading of OA severity. IPMC’s technologists are trained in proper weight-bearing positioning to ensure that your study provides the most clinically accurate information.
For a more detailed assessment of early joint space narrowing, a Rosenberg view (weight-bearing with the knees slightly bent at approximately 45 degrees) can be added. This view opens up the posterior aspect of the tibiofemoral joint where early cartilage loss often begins — and can reveal significant narrowing that looks normal on the standard straight-knee standing view.
When Does a Doctor Order a Knee X-Ray for Arthritis?
Your doctor may recommend knee X-ray imaging if you are experiencing:
- Chronic knee pain that worsens with activity and improves with rest — the classic OA symptom pattern
- Morning stiffness in the knee that resolves within 30 minutes (lasting more than 30 minutes suggests inflammatory arthritis rather than OA)
- A sensation of grinding, catching, or clicking in the knee with movement (crepitus)
- Knee swelling that comes and goes with activity
- Reduced knee range of motion or difficulty straightening the leg fully
- Knee deformity — a bow-legged or knock-kneed appearance that has developed or worsened over time
- Pain at the front of the knee with stairs, squatting, or rising from a chair (suggesting patellofemoral involvement)
- Pre-operative assessment before planned knee replacement surgery
- Monitoring known OA — serial X-rays to track progression or assess treatment response
How to Prepare and What to Expect
A knee X-ray requires no preparation. You can eat, drink, and take your medications as normal. For complete guidelines, see IPMC’s X-ray preparation page.
Wear comfortable clothing that allows easy access to your knee. You will be asked to remove metal objects near the knee. For weight-bearing views, you will stand in front of the X-ray detector with your weight evenly distributed on both feet. The technologist will carefully position your feet and knees in the correct rotation to ensure the joint space is accurately measured.
A standard knee series for arthritis evaluation typically includes an AP (standing, front-facing) view, a lateral view (from the side), and a sunrise/skyline view (for the kneecap). A Rosenberg view may be added when early or subtle joint space narrowing is suspected. The entire exam takes approximately 10 to 15 minutes and is completely painless.
There is no recovery time. You can drive and return to all normal activities immediately after the exam.
When Is MRI Needed in Addition to X-Ray?
A knee X-ray is typically sufficient for diagnosing and staging osteoarthritis and for surgical planning purposes. However, there are situations where your doctor may order an MRI of the knee in addition to or instead of X-ray:
- When the X-ray looks normal but significant symptoms persist — MRI can detect early cartilage damage, bone marrow edema, and other structural changes before they become visible on X-ray
- When a meniscal tear or ligament injury is suspected alongside the arthritis — MRI evaluates soft tissues that X-ray cannot see
- When the diagnosis is uncertain and inflammatory arthritis (such as rheumatoid arthritis) or other causes need to be distinguished from OA
- In younger patients with early symptoms where understanding the true extent of cartilage damage has important long-term treatment implications
For most patients with typical knee OA symptoms and confirmatory X-ray findings, MRI is not required before initiating conservative treatment.
After Your Knee X-Ray: Results and Treatment Options
A board-certified radiologist at IPMC reviews every image, assigns the Kellgren-Lawrence grade for each compartment, and prepares a detailed report for your referring physician — typically within 24 to 48 hours. Your doctor will discuss the findings and recommend a treatment plan based on the severity of arthritis, your symptoms, functional limitations, and overall health.
Treatment options for knee OA span a wide spectrum depending on grade and symptoms. For milder disease (KL 1–2), the focus is on slowing progression and managing symptoms — weight management, physical therapy, strengthening exercises, and anti-inflammatory medications. For moderate disease (KL 3), corticosteroid or hyaluronic acid injections, bracing, and activity modification become more prominent. For severe disease (KL 4) that does not respond to conservative measures, a surgical consultation for total or partial knee replacement is typically discussed.
Serial knee X-rays — repeated at 1-to-2-year intervals — allow your doctor to track how quickly the arthritis is progressing and adjust the treatment plan accordingly. If you are approaching the threshold for surgery, documented progression on X-ray provides important supporting evidence.
X-rays at IPMC
Why Choose IPMC for Your Knee X-Ray in Philadelphia?
Proper Weight-Bearing Technique Every Time
Accurate OA staging depends on weight-bearing X-rays taken with precise positioning. IPMC’s technologists are trained in standing knee X-ray protocols — including Rosenberg views when needed — ensuring your images provide the most clinically reliable joint space measurements and the most accurate Kellgren-Lawrence grade.
Board-Certified Radiologists
Every knee X-ray is interpreted by a board-certified radiologist who assigns a formal Kellgren-Lawrence grade for each compartment. Detailed reports — including grading, compartment-specific findings, and alignment assessment — are sent directly to your referring physician within 24 to 48 hours.
Fast Appointments, No Hospital Wait Times
Most knee X-ray appointments at IPMC are completed in about 10 to 15 minutes. Same-day and next-day scheduling is often available. When you need imaging for knee pain evaluation or pre-surgical planning, you shouldn’t have to wait weeks for a hospital appointment slot.
Convenient Location and Flexible Hours
Located at 9908 E. Roosevelt Blvd. in Northeast Philadelphia with onsite parking. Open Monday–Friday, 8AM–8PM. We accept most major insurance plans.
Schedule Your Knee X-Ray at IPMC in Philadelphia
If your doctor has recommended a knee X-ray for osteoarthritis in Philadelphia, IPMC provides fast, accurate weight-bearing imaging in a comfortable outpatient setting in Northeast Philadelphia — with results and a formal Kellgren-Lawrence grade delivered directly to your physician.
- Call 215-464-3300 to schedule your appointment.
- 9908 E. Roosevelt Blvd., Philadelphia, PA 19115
- Monday–Friday, 8AM–8PM