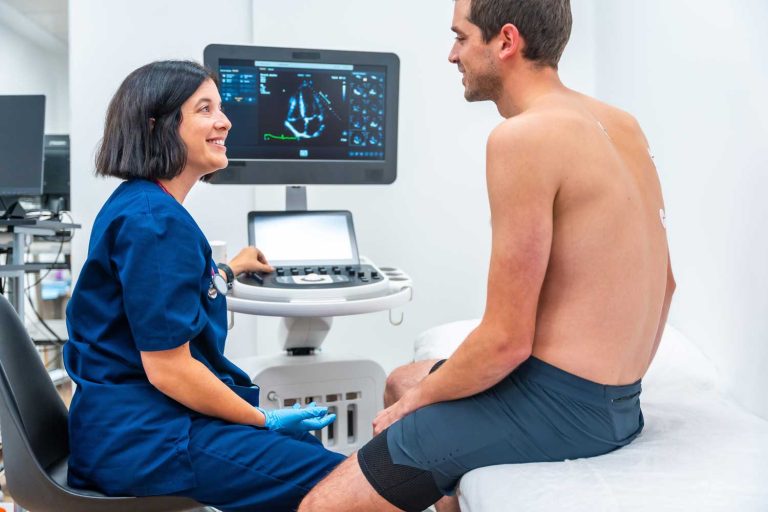
A stress echocardiogram — commonly called a stress echo or stress echo test — is one of the most informative and widely used cardiac tests available. It combines two established tools — an echocardiogram (ultrasound of the heart) and a physical stress test (exercise on a treadmill) — to reveal how your heart muscle and valves perform not just at rest, but under the demands of exercise. Because many heart problems only become apparent when the heart is working hard, this dual-view approach is far more revealing than either test alone.
Stress echocardiography is completely non-invasive and radiation-free. It uses only sound waves to image the heart — making it safer for many patients than nuclear stress tests or CT angiography, and repeatable without cumulative risk.
At Independent Physicians Medical Center (IPMC) in Northeast Philadelphia, our dedicated cardiology center offers stress echocardiography performed by experienced cardiac sonographers and interpreted by board-certified cardiologists — all in a comfortable outpatient setting without hospital wait times.
What Is Stress Echocardiography and How Does It Work?
A stress echocardiogram works by capturing ultrasound images of your heart in two states: at rest and immediately after peak exercise. Comparing these two sets of images allows your cardiologist to identify areas of the heart that are not receiving adequate blood flow — a key sign of coronary artery disease (CAD) — and to evaluate how well the heart’s valves and chambers function under real physiological demand.
Here’s the underlying physiology: when you exercise, healthy coronary arteries dilate to deliver more blood to the working heart muscle. When an artery is partially blocked by plaque (atherosclerosis), it cannot dilate adequately — and the segment of heart muscle it supplies begins to contract abnormally. This wall motion abnormality is visible on the echocardiogram immediately after exercise, even if the heart looked completely normal at rest.
According to the American Heart Association, stress echocardiography is an established, accurate test for coronary artery disease with sensitivity and specificity comparable to nuclear stress imaging — but without the radiation exposure.
Stress Echo vs. Resting Echo vs. Standard Stress Test: Key Differences
Patients are often confused about the differences between related cardiac tests. The table below clarifies what each test does and doesn’t show.
| Stress echocardiogram | Resting echocardiogram | Standard stress test (ECG only) | |
|---|---|---|---|
| What it measures | Heart structure + wall motion + valve function at rest AND under exercise stress | Heart structure, wall motion, valve function, ejection fraction — at rest only | Heart rate, blood pressure, and ECG changes during exercise — no imaging |
| Detects blockages (CAD) | Yes — directly via wall motion | Only if visible at rest (severe) | Indirectly via ECG changes |
| Sees valve function | Yes — at rest and under stress | Yes — at rest only | No |
| Radiation | None | None | None |
| Requires exercise | Yes (or medication if unable) | No | Yes |
| Approximate duration | 45–60 minutes total | 30–60 minutes | 30–60 minutes |
| Best for | Diagnosing CAD, evaluating chest pain, assessing valve disease under stress, pre-surgical cardiac risk | Evaluating heart structure, ejection fraction, valve disease, heart failure at rest | Screening for CAD, evaluating exercise capacity and ECG response |
If you cannot exercise due to joint problems, mobility limitations, or severe lung disease, a pharmacological (chemical) stress echo uses medication — typically dobutamine — to increase your heart rate and mimic the cardiovascular effects of exercise, allowing the same diagnostic information to be obtained without a treadmill.
What Does Stress Echocardiography Diagnose and Why Is It Ordered?
Your cardiologist or primary care doctor may recommend a stress echo for any of the following reasons:
Chest pain or pressure. The most common reason. A stress echo can determine whether symptoms are caused by reduced blood flow to the heart (ischemia) from coronary artery blockages — or whether the heart functions normally under exertion, pointing toward a non-cardiac cause.
Shortness of breath with activity. When breathlessness occurs during exercise, a stress echo helps determine whether the cause is cardiac — impaired pumping, ischemia, or valve disease worsening under load — or pulmonary and non-cardiac.
Known or suspected coronary artery disease (CAD). The test identifies which areas of the heart muscle are at risk from blockages, guides the decision between medical management and further workup (cardiac catheterization), and tracks progression of known disease over time.
After a heart attack. A stress echo assesses how much heart muscle remains healthy and whether residual blockages are causing ongoing ischemia — key information for planning rehabilitation and any additional intervention.
Abnormal resting ECG or inconclusive prior stress test. Imaging provides direct evidence of whether ECG changes represent true ischemia or a false positive — particularly valuable in patients with left bundle branch block (LBBB) or other baseline ECG abnormalities that make standard stress ECG interpretation unreliable.
Heart valve disease. Aortic stenosis and mitral regurgitation that appear manageable at rest may become hemodynamically significant during exercise. A stress echo evaluates how valve severity changes under load and helps guide the timing of intervention.
Cardiac risk factors and pre-operative assessment. Patients with diabetes, hypertension, high cholesterol, or a strong family history of heart disease may need baseline functional cardiac assessment before starting an exercise program or undergoing major non-cardiac surgery. A stress echo provides this functional data without radiation.
Unexplained palpitations or monitoring of known heart disease. A stress echo can reveal whether exercise-triggered palpitations coincide with ischemia or a structural abnormality, and serves as a reliable tool for tracking how the heart responds to medications, lifestyle changes, or prior cardiac procedures over time.
How to Prepare for Your Stress Echo at IPMC
Preparation for a stress echocardiogram is more specific than for a resting echo. Our full stress echo preparation guide has complete instructions. The key points:
Caffeine — avoid for 24 hours. This is the most critical preparation step. Avoid all caffeine for at least 24 hours before the test, including coffee, tea (including decaffeinated), soda, chocolate, and energy drinks. Caffeine interferes with the test’s ability to accurately assess your heart’s response and can produce false-negative results.
Beta-blockers — check with your doctor. Do not take beta-blockers on the morning of the test unless your doctor specifically instructs you to continue them. Beta-blockers slow the heart rate and may prevent you from reaching the target heart rate needed for a diagnostic result. Never stop any medication without first confirming with your prescribing physician.
Food and drink. Avoid a heavy meal for 3–4 hours before the test. Light eating is generally fine — an empty stomach is more comfortable during treadmill exercise. Stay well hydrated with water.
Other medications. Take all other medications as usual unless your doctor advises otherwise. Bring a complete list of current medications to your appointment.
Clothing and footwear. Wear comfortable exercise clothing and supportive athletic shoes with laces — you will walk on a treadmill. Avoid dresses, skirts, or restrictive clothing. A front-opening gown will be provided for electrode and transducer placement. Avoid smoking and alcohol for at least 3 hours before the test.
What Happens During a Stress Echocardiogram at IPMC?
The stress echo follows a consistent sequence of five phases:
- Preparation and baseline measurements. ECG electrodes are attached to your chest for continuous heart rhythm monitoring. A blood pressure cuff is placed on your arm. Your weight, height, and resting blood pressure are recorded to calculate your target heart rate (typically 85% of your age-predicted maximum: 220 minus your age).
- Resting echocardiogram. You lie on your left side on an exam table. A cardiac sonographer applies ultrasound gel to your chest and uses a transducer to capture detailed images of your heart from multiple angles — the four chambers, all segments of heart muscle, and each valve. These resting images establish your baseline for comparison. A resting ECG is also recorded.
- Treadmill exercise. You walk on a treadmill following a standardized protocol (the Bruce protocol is most common), in which speed and incline increase every three minutes. Your heart rate, blood pressure, and ECG are monitored continuously. You walk until you reach your target heart rate, develop significant symptoms (chest pain, severe shortness of breath, dizziness), or the test needs to be stopped for safety. Most patients exercise for 8–12 minutes. Tell the team immediately if you feel chest pain, pressure, dizziness, or any unusual discomfort.
- Post-exercise echocardiogram. Immediately after you step off the treadmill (within 60–90 seconds, while your heart rate is still elevated), you lie back down and the sonographer rapidly acquires another full set of echocardiogram images. This timing is critical — wall motion abnormalities caused by reduced blood flow are most visible in this immediate post-exercise window before the heart recovers.
- Recovery. You rest while your heart rate and blood pressure return to normal. The team continues monitoring your ECG until readings stabilize. Most patients feel fully recovered within 10–15 minutes.
The total appointment takes approximately 45 to 60 minutes. There is no recovery time — you can drive and return to normal activities the same day, unless your doctor advises otherwise based on your results.
Understanding Your Stress Echo Results
After the exam, a board-certified cardiologist reviews your resting and stress echocardiogram images side by side, alongside your ECG data and blood pressure response. Results are reported to your referring physician, who will discuss the findings and recommended next steps with you.
| Result | What it means | Typical next steps |
|---|---|---|
| Normal | All segments of the heart muscle contract normally and strengthen appropriately with exercise. No wall motion abnormalities. Adequate heart rate achieved. Blood pressure responds normally. | Coronary artery disease is unlikely as the cause of symptoms. Your doctor will discuss other possible causes and may recommend lifestyle modifications or continued monitoring. |
| Abnormal — new wall motion abnormality | One or more segments of the heart wall stop contracting normally or become weak during exercise — a sign that blood flow to that area is reduced, most commonly due to a coronary artery blockage. | Further evaluation typically includes coronary angiography (cardiac catheterization) or CT coronary angiography to identify and characterize the blockage. Treatment may include medication, stenting, or bypass surgery depending on severity. |
| Abnormal — reduced ejection fraction | The heart’s overall pumping function weakens with exercise rather than strengthening — indicating impaired cardiac reserve, possibly from cardiomyopathy or multi-vessel CAD. | Cardiology referral for further workup, possible cardiac MRI, and medication optimization or intervention planning. |
| Equivocal / inconclusive | Results are not clearly normal or abnormal — may occur if target heart rate was not achieved, image quality was limited, or findings are borderline. | Your doctor may recommend a repeat test with different protocol, pharmacological stress echo, nuclear stress test, or coronary CT angiography for a definitive answer. |
| Normal with valve finding | No ischemia detected, but a valve abnormality (e.g., mitral regurgitation worsening with exercise) is identified — which may itself explain symptoms. | Cardiology follow-up with possible repeat resting echocardiogram to monitor valve disease progression. |
Is a Stress Echo Safe? Risks and Contraindications
Stress echocardiography is considered a very safe test. It is performed under direct medical supervision with continuous ECG and blood pressure monitoring, and emergency equipment is immediately available throughout. Risks are uncommon and primarily related to the exercise itself rather than the ultrasound imaging.
During exercise you may experience chest tightness, shortness of breath, fatigue, or occasional palpitations — these are expected responses to vigorous exertion and resolve quickly once you stop. Always tell the team immediately if you feel chest pain, pressure, dizziness, or anything unusual during the test.
Exercise can trigger temporary abnormal heart rhythms in some patients, which typically resolve as soon as the treadmill stops. Continuous ECG monitoring throughout the test allows the team to respond immediately if needed, and the test is stopped at the first sign of a safety concern.
The risk of a serious cardiac event during a stress echo is very low — estimated at fewer than 1 in 10,000 appropriately selected patients. The test is not performed in patients with unstable angina, a heart attack within the past two days, severe uncontrolled arrhythmia, acute myocarditis or pericarditis, severe symptomatic aortic stenosis, decompensated heart failure, acute pulmonary embolism, or severely uncontrolled hypertension. Your cardiologist reviews your full history before ordering the test to confirm it is safe and appropriate for you.
If you cannot exercise due to joint problems, mobility limitations, or severe lung disease, a pharmacological stress echo using dobutamine or a vasodilator agent delivers the same diagnostic information without a treadmill.
Nuclear Medicine at IPMC
Why Choose IPMC for Your Stress Echocardiogram in Philadelphia?
Dedicated Cardiology Center
IPMC’s cardiology team specializes in cardiac testing and imaging. Stress echocardiograms are performed by experienced cardiac sonographers and supervised and interpreted by board-certified cardiologists — with results sent promptly to your referring physician. Meet our cardiologists.
Radiation-Free Cardiac Imaging
Unlike nuclear stress tests, stress echocardiography uses only ultrasound — no radiation, no radioactive tracers. The test is completely safe to repeat when monitoring is needed over time.
Full Range of Cardiac Testing Under One Roof
If your stress echo warrants follow-up, IPMC offers resting echocardiography, standard stress testing, pharmacological stress testing, and stress echo services — all at one convenient Northeast Philadelphia location.
Convenient Location and Flexible Hours
Located at 9908 E. Roosevelt Blvd. in Northeast Philadelphia with onsite parking. Open Monday–Friday, 8AM–8PM. We accept most major insurance plans.
Schedule Your Stress Echo at IPMC in Philadelphia
If your physician has recommended a nuclear medicine imaging test — such as a nuclear stress test or another study to evaluate heart function and blood flow — Independent Physicians Medical Center is here to provide reliable, advanced nuclear imaging close to home in Northeast Philadelphia. Nuclear medicine uses a small, safe amount of radioactive tracer to help your doctor see how organs and tissues are functioning, including how blood flows through your heart.
- Call 215-464-3300 to schedule your appointment.
- 9908 E. Roosevelt Blvd., Philadelphia, PA 19115
At IPMC, we believe nuclear imaging should be personal, efficient, and coordinated with your overall care plan — helping you and your doctor make confident decisions about your heart and vascular health.