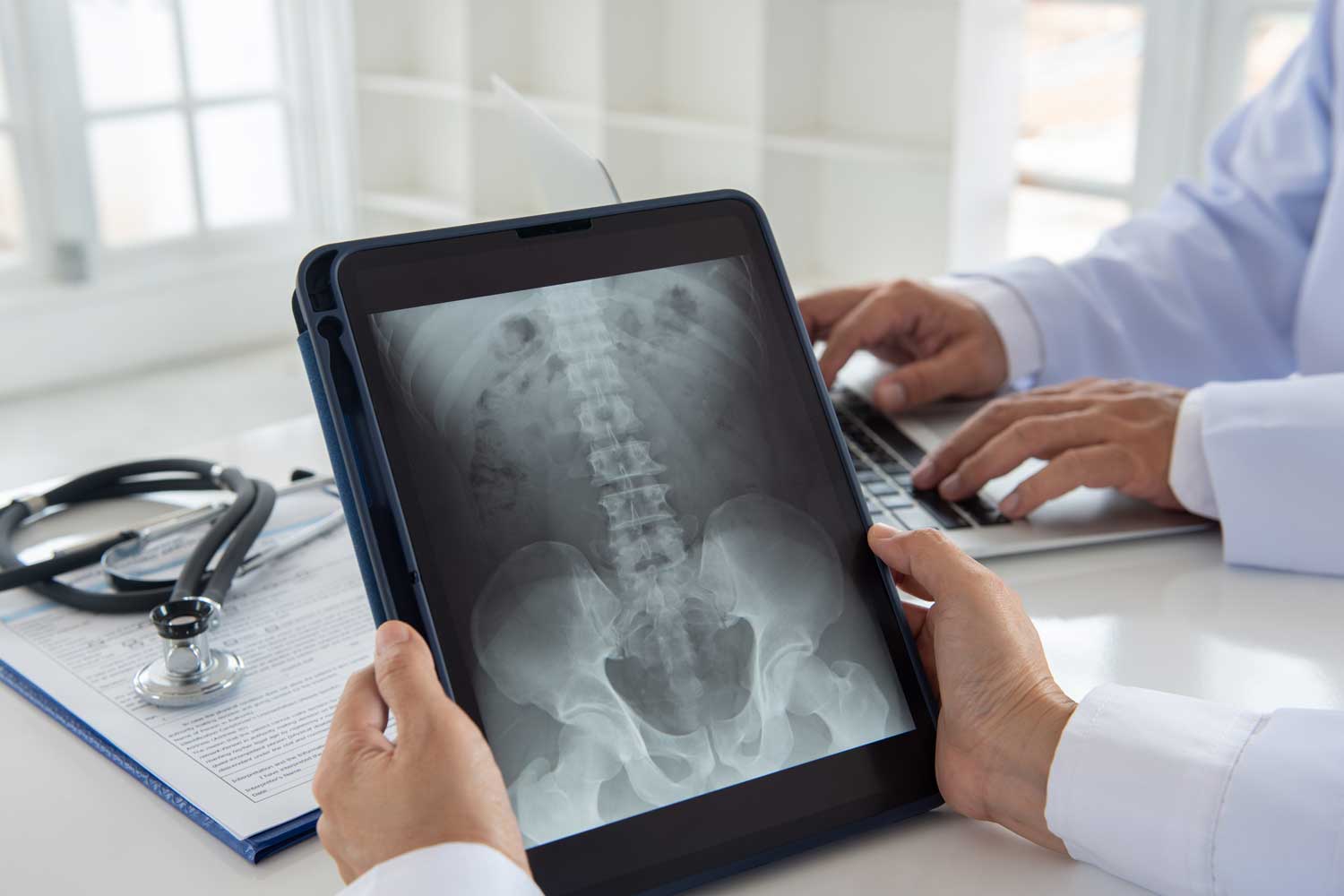
A pelvis X-ray — also commonly called a hip X-ray — is one of the most frequently ordered imaging studies in orthopaedics and emergency medicine. In a single fast, painless exam, it produces a comprehensive view of the pelvic bones, both hip joints, the sacrum, and the upper femurs, allowing your doctor to evaluate fractures, arthritis, joint alignment, and a wide range of other conditions affecting the hips and pelvis.
At Independent Physicians Medical Center (IPMC) in Northeast Philadelphia, we provide advanced digital pelvis and hip X-ray imaging using the Siemens Multix system — delivering sharp, high-resolution images in a comfortable outpatient setting with no hospital wait times. Learn more about our X-ray services.
Anatomy: What a Pelvis X-Ray Images
The pelvis is a bony ring made up of three pairs of fused bones on each side — the ilium (the broad upper blade), the ischium (the lower and back portion), and the pubis (the front lower portion). These three bones converge at the acetabulum, the deep socket that cups the rounded femoral head (the “ball” of the ball-and-socket hip joint). The two halves of the pelvis join at the front at the pubic symphysis and connect to the spine at the back through the sacroiliac (SI) joints, where the sacrum (the wedge-shaped bone at the base of the spine) articulates with each ilium.
A standard AP pelvis X-ray images all of these structures simultaneously — both hip joints, both sacroiliac joints, the pubic symphysis, the sacrum, and the upper femoral shafts — allowing direct comparison of the left and right sides and detection of subtle asymmetries that may indicate fracture, joint disease, or malalignment.
What Does a Pelvis X-Ray Show?
A pelvis X-ray can identify:
- Fractures — of the femoral neck, intertrochanteric region, pubic rami, acetabulum, sacrum, ilium, or ischium
- Hip dislocations — displacement of the femoral head from the acetabular socket
- Joint space narrowing — loss of the normal space between the femoral head and acetabulum, indicating cartilage loss from arthritis
- Osteophytes (bone spurs) — at the femoral head margins and acetabular rim, a hallmark of osteoarthritis
- Subchondral sclerosis and cysts — increased bone density and small cavities just beneath the joint surface, also indicating arthritis
- Sacroiliac joint changes — narrowing, sclerosis, or erosion of the SI joints, suggesting sacroiliitis or inflammatory arthritis
- Shenton’s line disruption — a smooth arc formed by the medial femoral neck and the superior pubic ramus; when this line is broken, it raises concern for a femoral neck fracture or hip dysplasia
- Avascular necrosis (AVN) — changes in the femoral head density indicating bone death from disrupted blood supply; early X-ray findings include subtle flattening and sclerosis of the femoral head
- Femoroacetabular impingement (FAI) — abnormal contact between the femoral head and acetabular rim due to bony morphology; visible as a “bump” on the femoral head (cam type) or over-coverage of the acetabulum (pincer type)
- Pubic symphysis abnormalities — widening (diastasis), erosion, or osteitis pubis (inflammation)
- Bone lesions and tumors — lytic (bone-destroying) or sclerotic (bone-forming) lesions in the pelvic bones or proximal femur
- Post-operative assessment — position and integrity of hip replacement hardware, pelvic screws and plates, or other orthopaedic implants
- Calcifications in soft tissues — vascular calcifications, phleboliths, or heterotopic ossification (abnormal bone formation in soft tissue)
Common Conditions a Pelvis X-Ray Diagnoses
Hip fractures. Hip fractures are one of the most consequential orthopaedic injuries, particularly in elderly patients. The most clinically important distinction is between intracapsular fractures (femoral neck fractures, within the joint capsule) and extracapsular fractures (intertrochanteric and subtrochanteric fractures, outside the capsule). Intracapsular fractures disrupt the blood supply to the femoral head and carry a significant risk of avascular necrosis and non-union; extracapsular fractures have better blood supply and generally heal more reliably. A pelvis X-ray with a lateral hip view is always the first imaging step. Note that some hip fractures — especially non-displaced femoral neck fractures in osteoporotic bone — can be occult on X-ray. If clinical suspicion is high and X-ray is negative, an MRI is the most sensitive follow-up study.
Hip osteoarthritis (OA). The hip is one of the most common sites for osteoarthritis, and a pelvis X-ray is the standard first imaging test. Classic findings include narrowing of the joint space (typically superior — the most weight-bearing area), osteophyte formation at the femoral head margins and acetabular rim, subchondral sclerosis, and subchondral cysts. Advanced OA may show superolateral migration of the femoral head and eventual bone-on-bone contact. Weight-bearing (standing) images provide the most clinically relevant information about joint space loss.
Pelvic fractures. High-energy trauma — motor vehicle accidents, falls from height — can fracture the pelvic ring. Pelvic ring fractures that disrupt both the anterior and posterior ring are unstable and can cause life-threatening haemorrhage. The AP pelvis X-ray is the standard initial trauma screen. For complex fractures requiring surgical planning, a CT scan provides far greater detail.
Sacroiliitis and ankylosing spondylitis. Inflammation of the sacroiliac joints is the hallmark of spondyloarthropathies — including ankylosing spondylitis, psoriatic arthritis, and inflammatory bowel disease-related arthritis. Early sacroiliitis may be subtle on X-ray (bilateral SI joint space narrowing, iliac-side sclerosis), but advanced disease produces progressive joint erosion, sclerosis, and eventually complete bony fusion (“bamboo spine”). X-ray has low sensitivity for early sacroiliitis; MRI is far more sensitive for detecting active inflammation.
Avascular necrosis (AVN) of the femoral head. AVN occurs when the blood supply to the femoral head is disrupted — from hip fractures, steroid use, alcohol, or other conditions. Early AVN may look normal on X-ray; later findings include a crescent sign (subchondral lucency from bone collapse), sclerosis, and eventual femoral head collapse. MRI is the most sensitive test for early AVN before X-ray changes appear.
Femoroacetabular impingement (FAI). FAI is a mechanical condition in which abnormal contact between the femoral head and the acetabular rim causes pain and damage to the cartilage and labrum — a common cause of hip pain in younger active adults. Two types are recognized: cam impingement (a non-spherical “bump” on the femoral head-neck junction) and pincer impingement (excess coverage of the femoral head by the acetabular rim). Both are identifiable on pelvis X-ray with specialist views.
Hip dislocation. Traumatic hip dislocation — most commonly posterior after a high-impact injury — is immediately visible on an AP pelvis X-ray as displacement of the femoral head from the acetabulum. Associated acetabular or femoral head fractures are common and require CT for full characterization.
Post-operative monitoring. Patients with hip replacement (total or partial), pelvic fixation hardware, or prior hip procedures are routinely followed with serial pelvis X-rays to assess implant position, detect hardware loosening or periprosthetic fracture, and monitor for complications.
When Does a Doctor Order a Pelvis X-Ray?
Common reasons your doctor may recommend a pelvis or hip X-ray include:
- Hip or groin pain after a fall, impact, or accident — to screen for fracture
- Inability or difficulty bearing weight after hip trauma
- Chronic hip or groin pain in adults — to evaluate for osteoarthritis, FAI, or other structural causes
- Lower back pain with buttock radiation — to evaluate the sacroiliac joints
- Morning stiffness and lower back pain in younger adults — to screen for sacroiliitis or ankylosing spondylitis
- Pre-operative planning before hip replacement surgery
- Post-operative follow-up after hip replacement or pelvic surgery
- Hip or pelvis pain in children — to evaluate for developmental dysplasia of the hip (DDH), Legg-Calvé-Perthes disease (avascular necrosis of the femoral head in children), or slipped capital femoral epiphysis (SCFE)
- Suspected bone lesion or tumor in the pelvis or proximal femur
- Groin or pubic pain in athletes — to evaluate for stress fractures of the pubic rami or femoral neck, or osteitis pubis
Views Taken During a Pelvis X-Ray
The AP (anteroposterior) pelvis view is the standard primary image — taken with the patient lying flat on their back and the X-ray beam directed from front to back. It shows both hips, the sacroiliac joints, the pubic symphysis, the sacrum, and the upper femoral shafts simultaneously. The legs are internally rotated 15–25 degrees to elongate the femoral neck, providing the best view of its anatomy. This symmetrical view allows direct side-to-side comparison and is the cornerstone of pelvic X-ray interpretation.
For suspected hip fracture, a lateral hip view of the affected side is always added. The most common lateral view for trauma is the cross-table lateral (horizontal beam lateral), which requires minimal movement of the injured hip — important because moving a hip with a suspected fracture can displace fragments. This view profiles the femoral neck and shows anterior-posterior displacement of fracture fragments that may not be apparent on the AP view alone.
Additional specialized views may be requested in specific situations. The frog-leg lateral is used in children (not in suspected fracture) to evaluate for Legg-Calvé-Perthes disease or slipped capital femoral epiphysis. Inlet and outlet views provide detailed assessment of the pelvic ring in complex trauma. Judet (oblique) views are used for acetabular fracture characterization. Your radiologist and referring physician will determine which combination of views is appropriate for your clinical situation.
How to Prepare and What to Expect
A pelvis or hip X-ray requires no preparation. You can eat, drink, and take your medications as normal. For complete guidance, see IPMC’s X-ray preparation page.
When you arrive, you will be asked to remove clothing with metal — belts, zippers, underwire bras — from the pelvic region, and to remove any jewelry. You may be given a hospital gown. You will lie on the X-ray table for the AP view; the technologist will position your legs and may place foam wedges under your heels to achieve the correct internal rotation.
Pregnancy: always inform the technologist if you are or may be pregnant. The pelvis X-ray directs the beam through the abdomen and pelvis, which includes the uterus. When the exam is medically necessary during pregnancy, the clinical benefit is weighed carefully against the radiation exposure, and shielding is used where feasible. Alternative imaging such as MRI (no radiation) may be considered depending on the clinical question.
The standard AP pelvis and lateral hip study takes approximately 10 to 15 minutes and is completely painless under normal circumstances. If you have a painful hip injury, the technologist will work carefully and minimize movement.
When Is MRI or CT Needed After a Pelvis X-Ray?
A pelvis X-ray is always the starting point — fast, inexpensive, and highly informative for most conditions. However, several situations call for follow-up cross-sectional imaging.
A CT scan is used when fracture anatomy needs to be defined in detail for surgical planning — complex pelvic ring fractures, acetabular fractures, and comminuted fractures of the proximal femur all require CT before operation. CT is also used in high-energy trauma when the plain X-ray may miss occult fractures, and to evaluate pelvic vasculature in the setting of traumatic haemorrhage.
An MRI is the investigation of choice when:
- A hip fracture is clinically suspected but the X-ray is normal — MRI detects occult femoral neck and pubic rami stress fractures with far higher sensitivity than plain X-ray
- Early avascular necrosis is suspected — MRI shows marrow signal changes weeks to months before X-ray changes appear
- Soft tissue pathology is the concern — labral tears, hip flexor injuries, bursitis, or gluteal tendon tears are invisible on X-ray and require MRI
- Early sacroiliitis is suspected — MRI with STIR sequences detects active inflammation in the SI joints years before X-ray findings appear
After Your Pelvis X-Ray: Results and Next Steps
A board-certified radiologist at IPMC reviews every image and sends a detailed written report to your referring physician, typically within 24 to 48 hours. Your doctor will explain the findings and recommend next steps, which may include:
- Orthopaedic referral and immobilization for a confirmed fracture
- Management recommendations for osteoarthritis, ranging from physical therapy and anti-inflammatory medications through to hip replacement discussion for severe disease
- CT or MRI for complex fracture planning or occult injury evaluation
- Rheumatology referral if sacroiliitis or inflammatory arthritis is identified
- Repeat X-rays at scheduled intervals to monitor arthritis progression, fracture healing, or implant position after hip surgery
- Reassurance that no significant bony abnormality is present
X-rays at IPMC
Why Choose IPMC for Your Pelvis X-Ray in Philadelphia?
Advanced Digital Imaging with the Siemens Multix
IPMC uses the Siemens Multix — a state-of-the-art digital radiography platform delivering sharp, high-resolution pelvis and hip X-ray images with minimal radiation. The Siemens Multix accommodates patients in a range of positions, including those with mobility limitations or hip injuries who need to remain supine throughout the exam.
Board-Certified Radiologists
Every pelvis X-ray is interpreted by a board-certified radiologist experienced in musculoskeletal imaging. Detailed reports — covering fracture assessment, joint space grading, SI joint evaluation, and recommendations for further workup — are sent directly to your referring physician within 24 to 48 hours.
Fast Appointments, No Hospital Wait Times
Most pelvis and hip X-ray appointments at IPMC are completed in under 15 minutes. Same-day and next-day scheduling is often available — so if you’ve had a recent hip injury, you can be seen and imaged quickly without the long waits of a hospital emergency or radiology department.
Convenient Location and Flexible Hours
Located at 9908 E. Roosevelt Blvd. in Northeast Philadelphia with onsite parking. Open Monday–Friday, 8AM–8PM. We accept most major insurance plans.
Schedule Your Pelvis or Hip X-Ray at IPMC in Philadelphia
If your doctor has recommended a pelvis X-ray in Philadelphia — for hip pain, a recent fall, or arthritis evaluation — IPMC provides fast, digital imaging in a comfortable outpatient setting in Northeast Philadelphia, with results delivered directly to your physician.
- Call 215-464-3300 to schedule your appointment.
- 9908 E. Roosevelt Blvd., Philadelphia, PA 19115
- Monday–Friday, 8AM–8PM