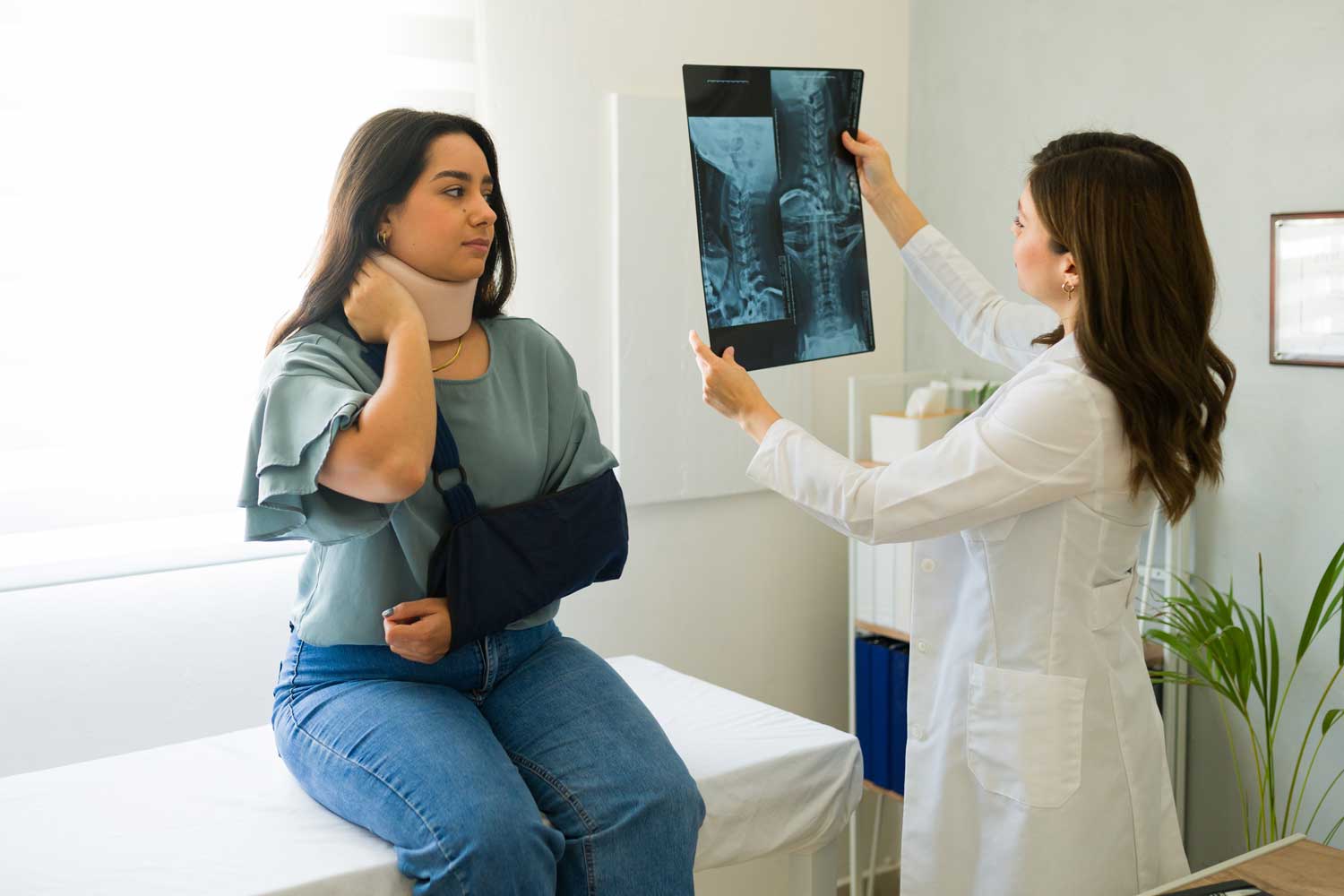
A neck X-ray — formally called a cervical spine X-ray or cervical spine radiograph — is the standard first-line imaging test for neck pain, injury, and stiffness. It produces detailed images of the seven cervical vertebrae (C1–C7), the disc spaces between them, the facet joints, and the overall alignment of the neck — giving your doctor essential information about fractures, arthritis, degenerative disc disease, and alignment abnormalities in a fast, painless exam.
At Independent Physicians Medical Center (IPMC) in Northeast Philadelphia, we provide advanced digital cervical spine X-ray imaging using the Siemens Multix system, with results typically available within 24 to 48 hours and sent directly to your referring physician. Learn more about our X-ray services.
What Does a Neck X-Ray Show?
The cervical spine is a complex structure: seven vertebrae, intervertebral discs, facet joints, and a network of ligaments — all compressed into a small space through which the spinal cord and the nerve roots to the arms pass. A cervical spine X-ray evaluates the bony architecture of this structure and provides important indirect clues about soft tissue conditions.
A neck X-ray can reveal:
- Fractures of the vertebral bodies, posterior elements (lamina, spinous processes), or the odontoid process (dens) of C2 — a critical structure for head and neck stability
- Dislocations and subluxations — vertebrae that have shifted out of alignment, which may indicate ligamentous injury and potential spinal cord risk
- Alignment abnormalities — including loss of the normal cervical lordosis (the gentle forward curve of the neck), which can indicate muscle spasm, injury, or degenerative disease
- Degenerative disc disease — narrowing of the intervertebral disc spaces, an indirect sign that the cushioning discs between vertebrae are thinning with age or wear
- Osteophytes (bone spurs) — bony projections at vertebral body edges or facet joints, a hallmark of cervical spondylosis (osteoarthritis of the cervical spine)
- Facet joint arthritis — narrowing and irregularity of the facet joints between adjacent vertebrae
- Prevertebral soft tissue swelling — widening of the soft tissue space in front of the vertebrae on the lateral view; a subtle but important sign of trauma-related bleeding or infection behind the throat
- Congenital abnormalities — including fused vertebrae (Klippel-Feil syndrome), transitional vertebrae, or other structural variants present from birth
- Scoliosis or kyphosis — abnormal lateral or forward curvature of the cervical spine
- Bone lesions and tumors — abnormal densities or destructive changes within vertebral bodies suggesting metastatic disease or primary bone tumors
An important limitation: a neck X-ray shows bones and bony changes well, but it does not directly visualize the spinal cord, nerve roots, or intervertebral discs (which are made of cartilage and fibrocartilage, invisible to X-rays). When soft tissue evaluation is needed — for herniated discs, nerve root compression, or spinal cord involvement — a cervical MRI scan is the appropriate next step.
Common Conditions a Cervical Spine X-Ray Diagnoses
Cervical fractures. A neck X-ray is the first-line study in trauma to detect vertebral fractures. Common fracture types include compression fractures of the vertebral body, posterior element fractures, odontoid (dens) fractures at C2, and the Jefferson fracture (a burst fracture of the C1 atlas). Widening of the prevertebral soft tissue on the lateral view — indicating bleeding behind the throat — is an important indirect sign of an underlying fracture or ligament injury that might otherwise be subtle. Because some fractures and ligamentous injuries can be missed on plain X-ray, a CT scan is often used for definitive trauma evaluation, particularly in high-energy mechanisms.
Cervical spondylosis (degenerative arthritis). The most common finding on cervical spine X-rays in adults over 50, cervical spondylosis reflects age-related wear and tear on the discs and facet joints. X-ray findings include narrowed disc spaces (especially at C5–C6 and C6–C7, the most mobile segments), osteophytes at vertebral body margins and facet joints, and endplate sclerosis. Spondylosis is a common cause of chronic neck pain and stiffness, and X-ray helps document its severity and distribution.
Cervical radiculopathy (pinched nerve). When osteophytes or narrowed disc spaces compress a nerve root exiting the spine, patients experience pain, tingling, or weakness radiating into the arm, shoulder, or hand — a pattern called cervical radiculopathy. A neck X-ray can show the bony degenerative changes contributing to this compression. However, X-ray cannot directly visualize the nerve or the disc itself; a cervical MRI is needed for definitive evaluation of nerve root compression.
Loss of cervical lordosis. The normal cervical spine has a gentle inward curve (lordosis) when viewed from the side. On X-ray, straightening or reversal of this curve (called “military neck” or kyphosis) can indicate acute muscle spasm from injury or pain, or underlying degenerative changes that have caused the spine to stiffen into an abnormal posture.
Whiplash-associated disorder. After a motor vehicle accident or other sudden neck injury, a cervical spine X-ray is typically the first imaging obtained to screen for fractures or instability. In many cases the X-ray is normal (whiplash primarily injures soft tissues, not bones), but it is an essential safety screen to exclude fracture before the patient is mobilized.
Instability. Flexion-extension views — X-rays taken with the neck bent forward and then extended — are used to assess dynamic alignment and detect ligamentous laxity or instability that may not be visible on static views. These views are only performed when the patient is neurologically intact and can move their neck voluntarily without significant pain.
Bone lesions and infection. Destructive changes to the vertebral body on X-ray may indicate spinal metastases, primary bone tumors, or spinal infections (discitis/osteomyelitis). These findings typically require further evaluation with MRI or CT.
When Does a Doctor Order a Cervical Spine X-Ray?
Common reasons your doctor may recommend a neck X-ray include:
- Neck pain after a fall, sports injury, motor vehicle accident, or direct blow
- Neck stiffness or reduced range of motion
- Chronic neck pain, especially in middle-aged or older adults in whom degenerative disease is suspected
- Pain, numbness, tingling, or weakness radiating into one or both arms or hands (cervical radiculopathy)
- Headaches originating at the base of the skull
- Suspected fracture after trauma
- Monitoring of known cervical spine conditions — including spondylosis, post-operative assessment, or scoliosis follow-up
- Pre-surgical planning or post-operative assessment of hardware position
- Suspected bone lesion or tumor in the cervical spine
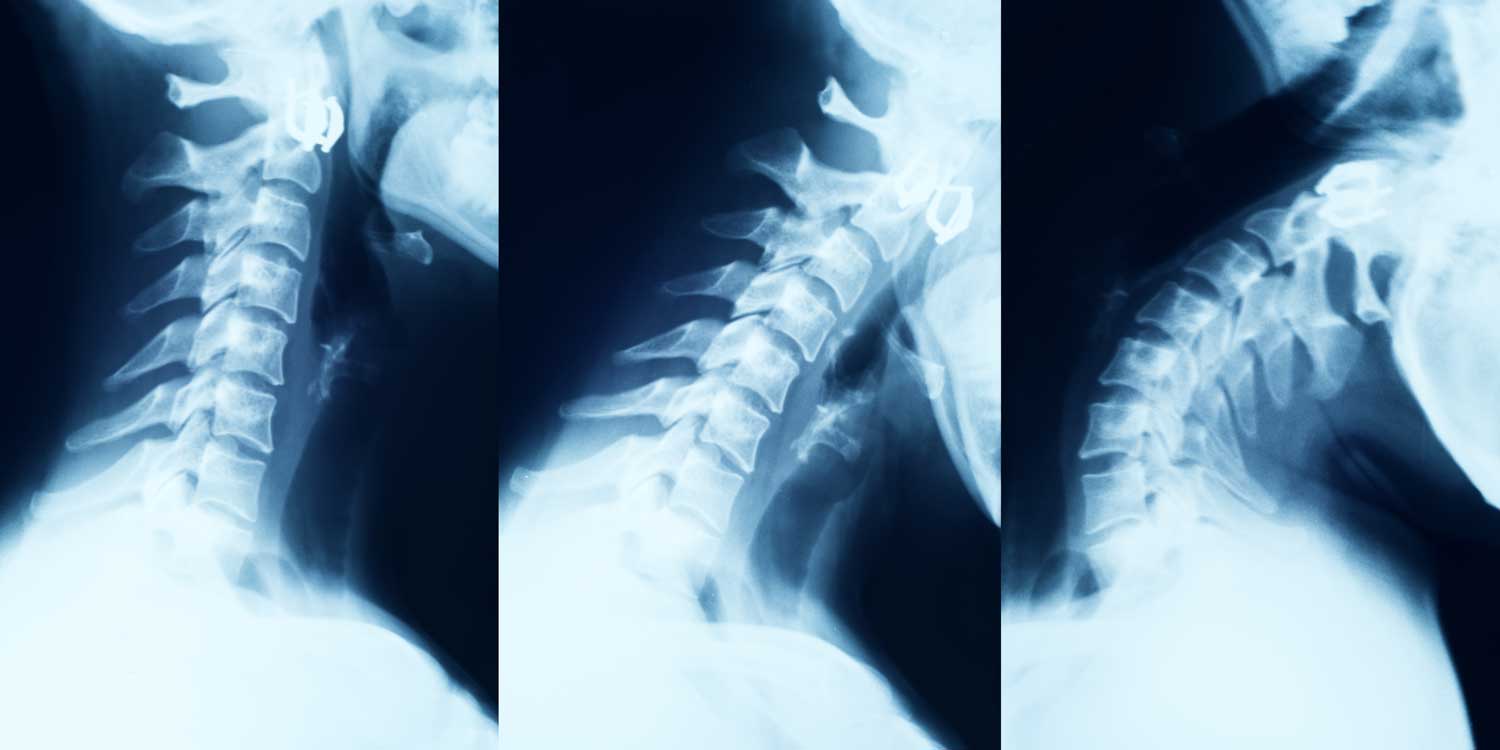
The lateral view is the most informative cervical spine X-ray projection, showing vertebral body alignment, disc space heights, the normal lordotic curve, and the prevertebral soft tissue — all critical for detecting fractures, degenerative disease, and instability.
Standard Views — and What Each One Shows
A standard cervical spine X-ray series consists of three to four views. Each provides distinct information that the others cannot.
The lateral view is the most informative single view of the cervical spine. Taken with the X-ray beam passing from one side of the neck to the other, it shows the vertebral bodies and disc spaces in profile, the overall curvature (lordosis), the four alignment lines that run along the anterior vertebral bodies, posterior vertebral bodies, spinolaminar line, and spinous process tips, and the prevertebral soft tissue. For the lateral view to be fully adequate, all seven cervical vertebrae must be visible down to the C7–T1 junction — if the shoulders obscure the lower vertebrae, a “swimmer’s view” with one arm raised is added.
The AP (anteroposterior) view is the frontal view taken with the beam passing from front to back. It shows the lateral alignment of the vertebral bodies, the spinous processes (which should form a straight line down the midline), and helps detect rotational malalignment, lateral disc space narrowing, and osteophytes at the vertebral margins.
The open-mouth odontoid view is taken with the mouth wide open and the beam passing through the open mouth. It provides an unobstructed view of the odontoid process (dens) of C2 and the C1–C2 joint — structures completely hidden behind the teeth and jaw on the standard lateral and AP views. It is essential for evaluating odontoid fractures and rotatory subluxation at the C1–C2 level.
Oblique views (taken at a 45-degree angle from either side) are used when the neural foramina need to be evaluated — these are the channels through which nerve roots exit the spine. Osteophytes or disc material encroaching into the neural foramen are better visualized on oblique views than on standard AP or lateral images.
How to Prepare and What to Expect
A cervical spine X-ray requires no preparation. You can eat, drink, and take your medications as normal. For complete preparation guidelines, see IPMC’s X-ray preparation page.
When you arrive, remove all jewelry from around your neck, including necklaces, earrings, and hairpins. Metal objects near the neck can create artifacts that obscure critical structures on the image. You do not need to change into a gown for most neck X-rays, though you should avoid wearing shirts with metal buttons or zippers near the collar.
You will stand, sit, or lie on a table depending on your clinical situation. Ambulatory outpatients are typically imaged standing or seated. For each view, the technologist will position your neck precisely and ask you to hold still for a fraction of a second during the exposure. For the open-mouth view, you will hold your mouth open as wide as possible.
Pregnancy: always inform the technologist if you are or may be pregnant. Cervical spine X-rays involve minimal scatter to the abdomen, but your care team will use appropriate shielding and confirm the exam is clinically necessary before proceeding.
The entire exam typically takes 10 to 15 minutes and is completely painless under normal circumstances. If your neck is injured and positioning is uncomfortable, the technologist will minimize movement and work with you carefully.
Cervical Spine X-Ray vs. MRI vs. CT: Which Does Your Doctor Choose?
The three main imaging options for the cervical spine have distinct strengths and are often used in sequence rather than as alternatives.
A neck X-ray is always the starting point — fast, low-cost, low radiation, and available immediately. It screens for fractures, evaluates overall alignment and curvature, and documents degenerative changes. For most patients presenting with acute neck pain or trauma, X-ray provides the initial assessment needed to guide further management.
A CT scan is used when the X-ray is inadequate (e.g., cannot visualize C7–T1), when a fracture is suspected but not definitively seen on X-ray, or when complex fracture anatomy needs to be defined for surgical planning. CT provides far more bony detail than plain X-ray and is the standard of care for high-energy trauma evaluation. IPMC offers CT imaging at the same convenient location.
A cervical MRI is the test of choice when the concern is soft tissue — herniated discs, nerve root compression (radiculopathy), spinal cord compression (myelopathy), ligamentous injury, or infection. MRI provides exquisite detail of the discs, nerve roots, spinal cord, and surrounding soft tissues that is simply invisible on both X-ray and CT. If your symptoms include radiating arm pain, progressive weakness, or coordination problems, your doctor will likely order an MRI in addition to or instead of plain X-rays.
After Your Cervical Spine X-Ray: Results and Next Steps
A board-certified radiologist at IPMC reviews every image and prepares a detailed written report for your referring physician, typically within 24 to 48 hours. Your doctor will explain the findings and discuss next steps.
Depending on what the X-ray shows, next steps may include:
- Reassurance and conservative management (physical therapy, anti-inflammatories, heat/ice) if no significant abnormality is found
- Immobilization and orthopedic referral if a fracture is identified
- A cervical MRI for further evaluation of disc disease, nerve root compression, or spinal cord involvement not visible on X-ray
- A CT scan for definitive fracture characterization or complex bony evaluation
- Specialist referral — to an orthopedic spine surgeon, neurosurgeon, or neurologist depending on findings and symptoms
- Repeat X-rays at a follow-up interval to monitor spondylosis progression or healing of a known fracture
X-rays at IPMC
Why Choose IPMC for Your Neck X-Ray in Philadelphia?
Advanced Digital Imaging with the Siemens Multix
IPMC uses the Siemens Multix digital radiography system — delivering sharp, high-resolution cervical spine X-ray images with minimal radiation. The Siemens Multix can accommodate patients in standing, seated, and recumbent positions, including those with injury-related mobility limitations.
Board-Certified Radiologists
Every cervical spine X-ray is interpreted by a board-certified radiologist with expertise in musculoskeletal and spine imaging. Detailed reports — covering alignment, fracture assessment, degenerative changes, and recommendations for further workup — are sent directly to your referring physician within 24 to 48 hours.
Fast Appointments and Same-Day Access
Most cervical spine X-ray appointments at IPMC are completed in 10 to 15 minutes. Same-day and next-day scheduling is often available — so if you’ve had a recent neck injury or your doctor needs urgent imaging, you don’t have to wait days for a hospital appointment.
Convenient Location and Flexible Hours
Located at 9908 E. Roosevelt Blvd. in Northeast Philadelphia with onsite parking. Open Monday–Friday, 8AM–8PM. We accept most major insurance plans.
Schedule Your Neck X-Ray at IPMC in Philadelphia
If your doctor has recommended a cervical spine X-ray in Philadelphia, IPMC provides fast, digital imaging in a comfortable outpatient setting in Northeast Philadelphia — with results delivered directly to your physician.
- Call 215-464-3300 to schedule your appointment.
- 9908 E. Roosevelt Blvd., Philadelphia, PA 19115
- Monday–Friday, 8AM–8PM